






Effective communication can make all the difference. Sometimes it is the simplest things – the right word of reassurance at the right time, or having your partner actively included in a care conversation can be highly effective ways to build and enhance the doctor-patient therapeutic relationship. Many clinicians do this incredibly well but there is always room for improvement. Experts from the VCCC Alliance have designed a new online education program for clinical staff to practice and refine their patient communication skills.
The program gives an overview of effective communication, while also providing experiential practice in the challenging area of palliative care and end-of-life conversations. An innovative virtual-reality teaching module combines instructional theory with fully simulated patient interview activities.
It is hoped that clinical staff, especially those working in supportive and palliative care, chronic pain management, and end-of-life care, as well as general practice, nursing and allied health undertake the self-paced learning either individually, or in small work-groups.
Palliative care is a growing area of health provision. Keeping pace with rapid change and demand for services requires a highly skilled workforce. People also need to be able to learn outside regular working hours and access up-to-the-minute information in community and regional settings, as well as the major hospitals. The new course is designed to meet this need.
It is the brainchild of a multidisciplinary team from Peter MacCallum Cancer Centre, St Vincent’s Hospital Melbourne, The Royal Melbourne Hospital, Western Health, Bendigo Health and the University of Melbourne. Former and current patients; men and women, young and old, from a range of backgrounds, who are passionate about sharing their experiences to improve things for others, have generously given their time to the project.
Course co-creator, Dr David Kok says that by practicing whenever and wherever they want, clinicians and health professionals will refine their skills to become better and more comfortable with communicating, especially in challenging situations.
Five communication modules are freely available. Prospective students can access the course according to their personal schedule, taking time to absorb and practice proposed strategies between each session.
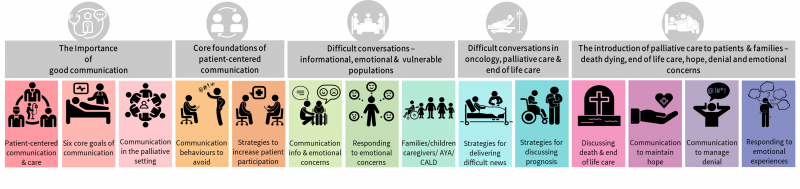
Image: Effective Communication in Patient Care – five modules each with multiple topics and activities
Peter Mac Senior Clinical Psychologist, Justine Diggens is the primary instructor on the course. “It was so enjoyable to be reminded of the simple ways in which effective communication can have such a positive impact on the quality of care provided to people with cancer and their families, particularly at vulnerable moments for them such as when difficult news needs to be discussed.
“It was wonderful to develop the modules with a collaboration of such a diverse team of clinicians as well as people with lived experience of cancer.”
“Effective communication can have such a positive impact on the quality of care provided to
people with cancer and their families, particularly at vulnerable moments for them.”
Features of the course include evidence-based patient case studies, patient stories and perspectives, interactive theoretical content, discussion boards, videos and animations. Content and activities provide around 40 hours of learning.
Effective Communication in Patient Care is available online via the VCCC Alliance website. Potential students are requested to register into the VCCC Learning Hub – a secure portal hosted on the University of Melbourne’s Canvas Learning Management System.
For more information on accessing the modules, contact VCCC Alliance Program Manager, Digital Interface, Erin Turner e: [email protected].
This project was sponsored by the VCCC Building Connectivity Program.
The project was developed by:
Dr David Kok – Radiation Oncologist, Director of Training, Peter MacCallum Cancer Centre, and VCCC Convenor, Master of Cancer Sciences
Ms Justine Diggens – Senior Clinical Psychologist, Peter Mac
Dr Daniel Sapkaroski – Radiotherapist and Clinical Educator, Peter Mac
Dr Sathana Dushyanthen – Medical Educator, University of Melbourne and VCCC
Project sponsors:
A/Professor Jennifer Weil – Deputy Director Palliative Care Medicine, Palliative Medicine Physician and Palliative Care Clinical Trials Lead, St Vincent’s Hospital Melbourne
Dr Alex Clinch, Peter Mac Palliative Care Consultant, Deputy Director Parkville Integrated Palliative Care Service - The Royal Melbourne Hospital and Peter MacCallum Cancer Centre
